About Mohs Surgery
Why Choose a Fellowship Trained Mohs Surgeon?
Mohs micrographic surgery has set a new standard in skin cancer treatment. An increasing number of physicians are performing Mohs surgery, which is now widely accepted as the most effective treatment for most types of skin cancer. However, not all Mohs surgeons receive the same level of training. Dr. Sharon Thornton has achieved the highest degree of Mohs surgery qualification by completing a two-year American College of Mohs Surgery approved fellowship. For you, this means peace of mind, knowing that you will receive superior quality and competency, as well as an optimal outcome. The ACMS (http://www.skincancermohssurgery.org/) was established by Dr. Frederic Mohs himself, and its fellowship training program is generally acknowledged as the benchmark in Mohs surgery training. Through an extensive application and interview process, only the most qualified physicians are selected by ACMS to participate in a fellowship program. Participants must undergo a rigorous 1 to 2 year training program subsequent to completing a residency in dermatology. During fellowship training, Dr. Sharon Thornton studied and trained under the guidance of veteran Mohs College surgeons who have demonstrated expertise in Mohs surgery. Since skin cancer occurs in a diversity of forms, degrees and locations, the ACMS fellowship program is set up to be thorough and stringent.
As an ACMS graduate, Dr. Sharon Thornton gained an uncommon level of exposure, including everything from challenging tumor locations to rare tumor pathology and complex wound reconstruction. She has the training and experience to achieve the best outcome from your skin cancer treatment.
Mohs Micrographic Surgery
Procedures & Treatments
Mohs Micrographic Surgery is a highly specialized state-of-the-art procedure for the precise removal of skin cancer. Guided by the microscope, the Mohs surgeon removes the skin cancer as a layer of tissue. This specimen is then mapped and microscope slides are processed and read by the Mohs Surgeon. 100% of the margins (both the deep and surrounding skin edges) are evaluated. No other surgical technique for the removal of skin cancer examines the entire margin of surrounding skin to ensure that the highest cure rate is obtained. If all margins are free of cancer, as examined under the microscope, the resultant skin defect is typically repaired that day. If a focal area demonstrates residual cancer, a second stage is taken only in the area that showed cancer cells, thereby preserving as much healthy tissue as possible. Again, microscope slides are made and read by the Mohs surgeon. This process continues until all margins are free of tumor. While every case is unique, Mohs surgery provides a cure rate up to 99% for primary skin cancers (those that have not been treated in the past). Please visit www.mohscollege.com for information about skin cancer and Mohs micrographic surgery.
Reconstruction
After a skin cancer is removed by Mohs micrographic surgery or an excision, the wound is repaired. Repair options are highly individualized. Dr. Thornton will thoroughly review wound repair options with each patient. In certain anatomic locations, sometimes the wound is left to heal on its own without stitches. There are specific criteria that allow a wound to heal well on its own. Frequently, a side-to-side closure with stitches is performed. If the wound will not close from side-to-side or if a side-to-side closure would be distorting, then a skin flap or skin graft is performed. A skin flap moves healthy skin adjacent to the wound over to cover the nearby wound. A skin graft is the transplantation of healthy skin from another anatomic location into the wound. Details of reconstruction are reviewed at length on the day of your surgery.
The Mohs Step-by-Step Process
The Mohs surgery procedure seems simple: the surgeon removes the cancer, carefully checks to be sure the he or she got it all, then repairs the wound. American College of Mohs Surgery members, however, train in and practice the complex nuances of this process for years so they are prepared to handle any situation they may encounter. This page describes the steps they follow for each Mohs surgical procedure.
Step 1

The roots of a skin cancer may extend beyond the visible portion of the tumor. If these roots are not removed, the cancer will recur. A surgery starts with the American College of Mohs Surgery (ACMS) specialist examining the visible lesion and planning what tissue to remove. The patient then receives local anesthesia, and the Mohs surgery begins.
Step 2
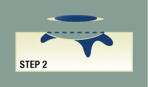
The surgeon removes the visible portion of the tumor using careful surgical techniques.
Step 3
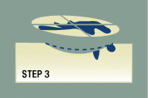
The ACMS surgeon next removes a deeper layer of skin and divides it into sections. With the help of technicians, the surgeon then color-codes each of these sections with dyes and makes reference marks on the skin to show the source of the sections. A map of the surgical site is then drawn to track exactly where each small portion of tissue originated.
Step 4
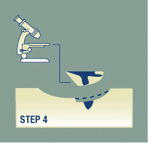
In a laboratory, the surgeon uses a microscope to examine the undersurface and edges of each section of tissue in search of evidence of remaining cancer.
Step 5
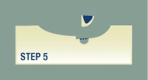
If the surgeon finds cancer cells under the microscope, he or she marks their location on the “map” and returns to the patient to remove another deeper layer of skin — but only from precisely where the cancer cells originated. This method ensures that the Mohs surgery results in the smallest scar possible.
Step 6
The removal process stops when there is no longer any evidence of cancer in the surgical site. Because Mohs surgery removes only tissue containing cancer, it ensures that the maximum amount of healthy tissue is kept intact.
At this point, the surgeon discusses reconstruction options, should they be required, and then post-operative care. Mohs surgery recovery tends to be easily manageable because of the use of local anesthesia and the careful surgical techniques.
Last updated: March 2, 2017
On the Day of Surgery
On the day of surgery, you will be asked to identify the surgical site (prior biopsy site). Please pay attention to the exact location of the biopsy prior to your visit.
On the day of surgery:
- Eat a light, healthy breakfast.
- Avoid alcoholic beverages 24 hours prior to surgery
- Take all of your medications as prescribed.
- Bring a list of all medications that you take (prescribed and over-the-counter). Please include dosage, frequency, etc.
- Bring lunch with you.
- You may want to bring reading materials, needlework, etc.
- We recommend a shower the evening or morning before your surgery and freshly laundered clothes to help reduce the risk of infection. Please wear a shirt that buttons up the front. Also, dress accordingly due to cooler office temperature settings.
- Do not apply make-up, cream, or shaving lotion, etc., to the affected area.
- Bring a container for contact lenses, dentures and hearing aids. Be prepared that you may need to remove these items prior to surgery.
- Avoid any after-surgery appointments because you may be in our office for an extended period of time.
- If you require supplemental oxygen, please bring enough to last approximately 6-8 hours.
A list of needed supplies for proper wound care following surgery will be included in your post-operative instructions. For your convenience, you have the option to purchase a wound care kit in our office at the conclusion of your surgery. If you choose to purchase a wound care kit, payment will be due at the time of your appointment. Otherwise, you may purchase wound care supplies at a local pharmacy.
Frequently Asked Questions
What is Skin Cancer?
Skin cancer, like other types of cancer, is the uncontrolled growth of abnormal cells. The three most common skin cancers are basal cell carcinoma, squamous cell carcinoma and melanoma. If caught early, skin cancer can be treated very effectively. Left untreated, the cancer will continue to grow and invade deeper tissues. Squamous cell carcinoma and melanoma may also spread throughout the body, or metastasize.
What is Mohs Surgery?
Mohs surgery is a highly specialized and effective office-based procedure used to treat skin cancer. It is named after Dr. Frederic Mohs, who pioneered the technique.
Mohs surgery allows the removal of the skin cancer in layers. The surgeon removes the visible tumor, draws a map to orient the tissue and inks the tissue before taking it to the on-site Mohs laboratory. The tissue is processed and then examined under the microscope. Any microscopic roots or extensions of the cancer are identified and mapped. If cancer is seen at the lateral or deep margin, an additional tissue layer is taken only in the area that is positive. Normal tissue is spared. Once the cancer is entirely removed, wound repair options are discussed and reconstruction is performed.
Do I need surgery after a biopsy?
Yes. Often the skin will look better after the biopsy because the biopsy may remove some or nearly all the visible tumor. However, cancer cells may remain at the site on the skin. Left untreated, these roots of the tumor can continue to grow deeper and wider. Mohs surgery enables the surgeon to evaluate 100% of the lateral and deep margin to make sure that the cancer is completely removed and no residual cancer cells are left behind in the skin.
What makes Mohs Surgery different than other types of surgery?
Mohs surgery has the highest cure rate for common sun-induced skin cancers and many other types of skin cancer. The surgery is performed with local anesthesia only and you will not need to be sedated or put to sleep. The tumor is removed with confirmation of clear margins at the time of the surgery. Normal healthy tissue surrounding the tumor is spared. Reconstruction of the wound can be performed the same day. Dr. Thornton completed a two-year fellowship in Mohs micrographic surgery and cutaneous oncology. During her fellowship, she trained under several excellent Mohs surgeons, including Dr. Philip Bailin, who learned Mohs surgery directly from Dr. Mohs himself.
Will my insurance cover the cost of surgery?
Under most circumstances, your health insurance company will pay for Mohs surgery. In some instances, it may be necessary to obtain a referral or authorization from your primary physician or insurance company prior to surgery. If you are in doubt about your particular coverage, it would be useful to check with your insurance representative prior to your appointment. If you have specific questions regarding insurance or billing matters, place contact our office (614) 389-2200.
How will my surgical wound be repaired?
Once the cancer is completely removed, wound repair options are thoroughly reviewed with Dr. Thornton. Sometimes, the wound is left to heal on its own without stitches. Other wound repairs that require stitches include side-to-side closure, a skin flap and a skin graft.
How long will my appointment and surgery last?
The length of time to remove the tumor depends on the size and extent of the tumor. Processing of the tissue in the lab during the surgery takes time as well. We recommend you plan to be in our office at least 3-4 hours. You will be in the waiting room with a pressure bandage applied to your wound while we are waiting on the tissue in the lab. Please bring snacks, lunch, reading materials, mobile devices, etc. We offer free Wi-Fi for mobile devices. A refrigerator and a microwave are available for your use in the waiting room.
Do I need to stop any of my medications prior to surgery?
No. We recommend that you continue to take all of your prescribed medications prior to surgery, including blood thinners.
Do I need antibiotics prior to surgery?
If you have been told that you need antibiotics prior to dental work or other surgical procedures, we may give you antibiotics to take prior to surgery. Please notify us while you are here the day of surgery.
How do I take care of my surgical wound?
The wound care will be reviewed after surgery based on the type of wound repair you have. We generally recommend no heavy lifting or aerobic activity for at least 1 week after surgery.
Will I have a scar after my surgery?
Yes, any treatment for skin cancer and surgery leaves a scar. Our goal is to leave the least mark possible on your skin. Mohs surgery preserves as much normal, healthy skin as possible.
Can I drive after surgery?
We prefer you plan to have a driver available after surgery, if possible. A driver will be especially important if the tumor is close to your eye where a bandage may obstruct your vision.
Where can I find out more about Mohs Surgery?
The American College of Mohs surgery has a very informative website at
www.skincancermohssurgery.com
If you have additional question prior to your surgery date, please do not hesitate to call our office at (614) 389-2200.
